How Autoimmune Conditions Affect Skin and Hair

Autoimmune conditions can affect skin and hair in many ways. Learn why symptoms appear and how gentle, supportive skincare can help protect the skin barrier.
Autoimmune conditions are often thought of as internal diseases. But for many people, the first signs appear on the outside.
Hair that suddenly sheds. Skin that becomes painfully dry. Rashes that refuse to calm down. Areas that feel tight, fragile, or inflamed.
These changes can feel confusing and deeply personal. Skin and hair are closely tied to how we see ourselves. When they change, confidence can shift too.
Understanding what is happening beneath the surface can make these changes easier to navigate. With the right knowledge and gentle care, many people find ways to support their skin and hair through these challenges.
Why Autoimmune Conditions Affect Skin and Hair
In autoimmune disease, the immune system mistakenly attacks healthy tissues in the body.
Sometimes this affects hair follicles.
Sometimes oil glands or moisture production.
Sometimes collagen, circulation, or hormone balance.
Because skin is the body’s largest organ—and hair follicles are sensitive to hormonal and immune shifts—changes often become visible there first.
These symptoms are not cosmetic. They are biological.

Hair Loss and Hair Texture Changes
Conditions in this group
- Alopecia areata
- Lichen Planopilaris (LPP)
- Hashimoto’s thyroiditis
- Graves’ disease
Hair loss is one of the most emotionally difficult symptoms many people experience. It can happen suddenly or gradually, and sometimes without warning.
Alopecia areata occurs when the immune system targets hair follicles, often causing round patches of hair loss.
Lichen Planopilaris (LPP) shows up as gradual hair thinning in affected patches accompanied by scalp inflammation.
Thyroid-related autoimmune conditions like Hashimoto’s thyroiditis and Graves’ disease disrupt hormone balance. These hormones play a major role in the hair growth cycle and oil production in the skin.
Common changes include:
- Hair thinning
- Increased shedding
- Dry, brittle strands
- Flaky or sensitive scalp
- Skin that feels dry or reactive
— Marie, 42, says
“When my Hashimoto’s flared, I noticed my hairbrush filling up faster than usual. My scalp became dry and itchy too. Learning to switch to gentler shampoo and conditioner bars helped my scalp calm down, and that made a big difference emotionally.”

Inflammatory Skin Conditions
Conditions in this group
- Psoriasis
- Discoid lupus
- Dermatitis herpetiformis
- Eczema
- Rosacea
- Contact dermatitis
- Hives (urticaria)
- Perioral Dermatitis
- Lupus Miliaris Disseminatus Faciei (LMDF)
These conditions involve inflammation and a disrupted skin barrier. The skin becomes reactive, sensitive, and sometimes painful.
Psoriasis causes thick, scaly plaques that may crack or itch.
Discoid lupus can create red, scaly lesions on the scalp or face that sometimes lead to hair loss.
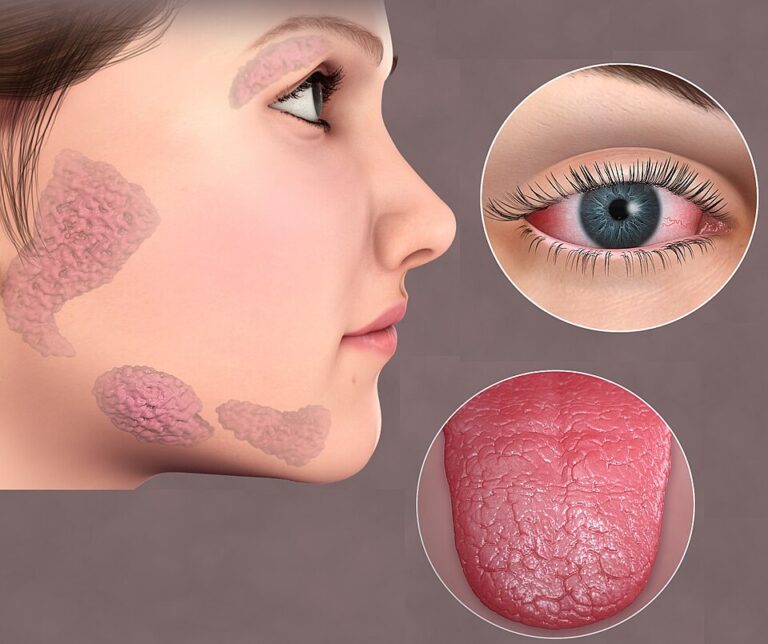
Lupus Miliaris Disseminatus Faciei (LMDF) affects the eyes, nose, and cheeks, with slightly scaly or crusted bumps.
Dermatitis herpetiformis, often linked to gluten sensitivity, causes intensely itchy blister-like rashes.
Eczema, rosacea, contact dermatitis, perioral dermatitis, and chronic hives may also occur alongside immune dysfunction.
Symptoms often include:
- Persistent itching
- Redness or inflammation
- Flaking or scaling
- Skin cracking or irritation
- Sensitivity to products
— Daniel, 37, says
“With psoriasis, my skin reacts to almost everything during a flare. Switching to natural soaps and avoiding synthetic fragrances helped calm the itching. It didn’t cure the psoriasis, but it made daily life much more comfortable.”
Skin Thickening and Structural Changes
Conditions in this group
- Scleroderma
- CREST syndrome
- Erythema nodosum
- Lichen sclerosus
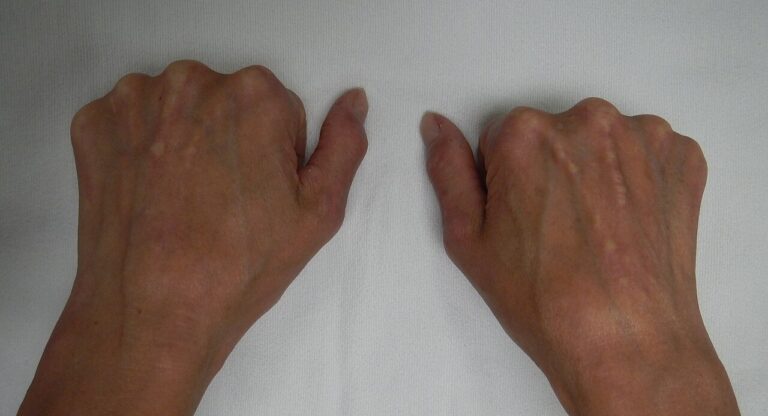
Some autoimmune conditions affect connective tissue and collagen, which changes the structure and flexibility of the skin.
Scleroderma can cause skin to become tight or hardened.
CREST syndrome, a form of limited scleroderma, also involves circulation changes that affect the skin.
Erythema nodosum appears as tender nodules under the skin, often on the legs.
Lichen sclerosus causes fragile skin that can become inflamed and easily irritated.
These conditions can make skin feel:
- Tight or stiff
- Painful or inflamed
- Fragile or easily irritated
— Anna, 51, says
“My lichen sclerosus makes my skin incredibly sensitive. Even clothing fabrics can trigger discomfort. Learning to use gentler skincare, like body butter, and avoid irritants helped me feel more in control.”
Extreme Dryness and Skin Barrier Challenges
Conditions in this group
- Sjögren’s disease
- Progesterone dermatitis
Some autoimmune diseases directly affect moisture production.
Sjögren’s disease is widely known for dry eyes and mouth, but it can also cause extremely dry skin.
Progesterone dermatitis can trigger cyclical flare-ups tied to hormonal changes.
When the skin loses moisture, the barrier weakens. This makes the skin more vulnerable to irritation, allergens, and environmental stress.
People often notice:
- Tight, uncomfortable skin
- Increased sensitivity
- Flaking or cracking
- Extremely dry and chapped lips
— Laura, 45, says
“Living with Sjögren’s means my skin dries out very quickly. Heavy creams and gentle soaps made a huge difference. It’s not perfect, but my skin feels calmer and less reactive.”
Common Allergen Triggers
Allergens trigger the immune system to defend against what it thinks is a threat. The body releases inflammatory chemicals, such as histamine. This can happen to anyone with an allergy.
For people with autoimmune disease, the immune system essentially becomes more stimulated than it should be, which can aggravate existing autoimmune reactions.
Environmental allergens
Pollen
Dust mites
Mold spores
Pet dander
Plant exposure
Poison ivy
Poison oak
Sumac
Metals
Nickel (jewelry, buttons, buckles)
Chemicals
Synthetic fragrances
Dyes
Parabens
Latex
Harsh detergents
Foods and medications
Certain foods
Antibiotics
Some prescription medications
When the immune system is already reactive, even small irritants can trigger larger skin responses.

Supporting Skin and Hair During Autoimmune Flares
Medical treatment should always be guided by a healthcare provider. But everyday care can still make skin feel more comfortable.
Helpful strategies include:
- Choosing gentle, fragrance-free cleansers
- Avoiding harsh detergents and alcohol-based products
- Using nourishing oils and butters
- Moisturizing on damp skin
- Avoiding known triggers
- Reducing friction on fragile areas
When skin is already under stress, the goal is not aggressive treatment.
It is protection.
Skin that feels safe often reacts less.
Living With Autoimmune Skin Changes
Autoimmune diseases are complex. They affect comfort, confidence, and daily routines.
But visible symptoms do not define you.
Many people discover that small, supportive habits—gentle cleansing, barrier-friendly moisture, and reducing irritants—can help their skin feel calmer over time.
Healing is rarely linear. Some days are easier than others.
On the harder days, the goal can simply be this:
Protect the barrier.
Reduce irritation.
Treat your skin with the same patience you would offer someone you love.

